Are Vaccines Africa’s Silver Bullet?
Author: Toriola Basit
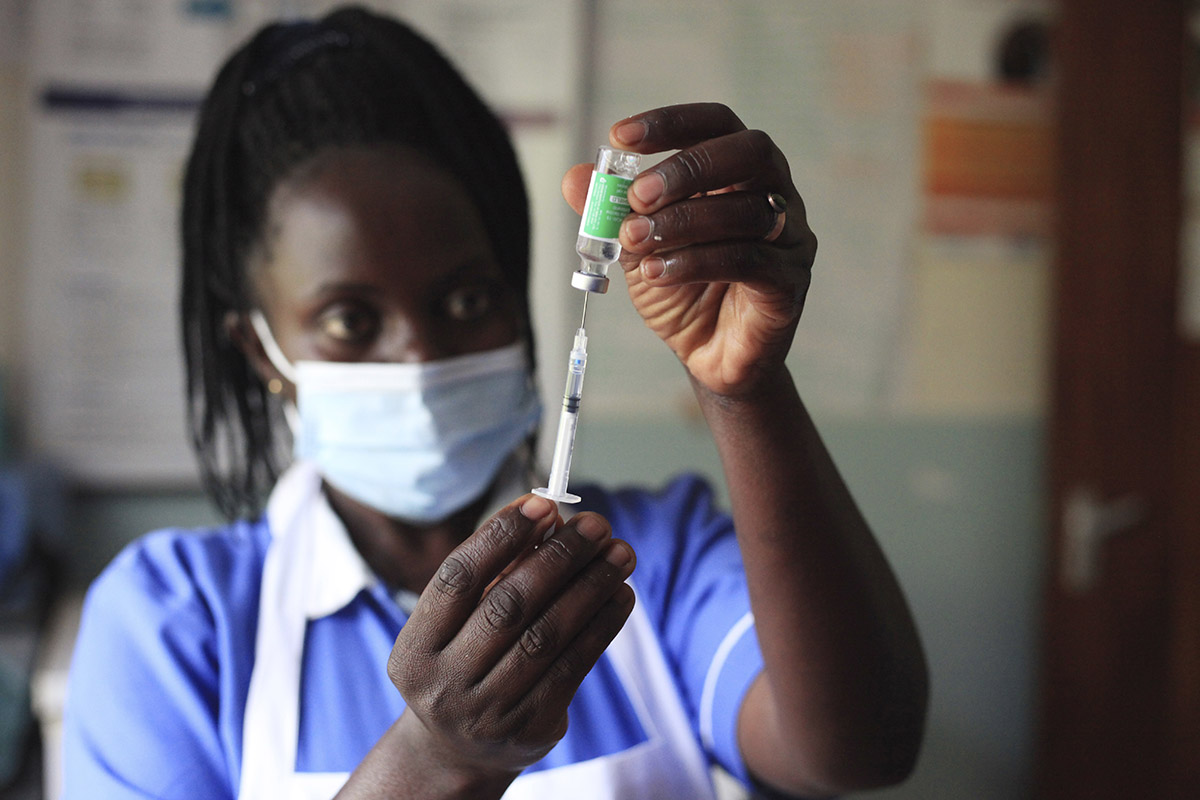
For decades now, Malaria has been a huge threat to children in Africa — it has killed half a million of our children every passing year. Did you know that on an average day, the disease accounts for the death of 1320 children? Or that, nearly every time the second hand of a wall clock counts to 60, a child somewhere in Africa succumbs to Malaria? [1]
You can only begin to imagine how African mothers would jump for joy if they heard about a vaccine that can cure the dreaded malaria. That was exactly the case in October 2021. The World Health Organisation (WHO) announced RTS, S as a Malaria vaccine recommended for broad use. It was historic!
Throughout Africa, the continent shouldering the heaviest Malaria burden, the vaccine offered a glimmer of hope and became a huge stepping stone in figuring out what vaccines will work better in the near future.
In December 2022, a newer vaccine was launched. It was named R21. This vaccine was described as more effective, and more potent than its predecessor — the RTS, S. After seeing the approval of the WHO and local health bodies, African countries such as Ghana, Liberia and Nigeria officially adopted R21 for broad use.
Since the vaccine’s approval, clinical trials and other studies have been ongoing to determine its effectiveness. R21 is now confirmed to reduce malaria symptoms by 75%. [2] At this efficacy, it is believed to have a “world-changing” potential.
Still, the R21 vaccine and other existing chemopreventive measures are no silver bullets — they do not have it all shiny and rosy. For this reason, we need to begin paying more attention to other underlying factors that have significantly contributed to the endemic spread of malaria.
Despite the fact that the Oxford team and the Serum Institute of India have promised to produce a whopping 200 million doses of R21 vaccines annually, accessing these vaccines is a major stumbling block to the efficiency of malaria vaccines in Africa. Most victims of Malaria live in poor and rural areas that are far away from local health centres. For instance, more than 3.1 million people in Nigeria are estimated to have either not completed or received a single dose in a national immunisation schedule. [3]
Also, malaria parasites are known to build up resistance and evade almost anything the host throws at them. In the past, P. falciparum, the most lethal malaria parasite species, restrained several chemopreventive drugs from working well. [4] Such drugs include chloroquine, quinine, and even artemisinin. This resistance has raised concerns about the future of the new malaria vaccines.
To beat malaria, we must target its parasite from all facets — whether in mosquitoes or infected humans. It is noteworthy that Malaria is preventable and curable if diagnosed early and prompt and effective treatment with artemisinin-based combination therapies are used. In fact, a few African countries like Mauritius (1973), Lesotho (2012), Algeria (2019), and Cabo Verde (2024) have successfully eliminated malaria by strengthening their health systems and increasing access to diagnosis and treatment of all cases. [5]
Since the vaccines are not 100% unfailing, they must be combined with personal protective measures. For instance, the simple act of destroying mosquito breeding grounds in stagnant water, employing Long-Lasting Insecticidal Bed Nets (LLINs), dressing in long-sleeved shirts and trousers, applying insect repellent to exposed skin—particularly at nights when mosquitoes are most active, using Indoor Residual Spraying (IRS), etc, will go a long way in curbing the spread of malaria.
Furthermore, malaria elimination and eventual eradication will require sustainable routine childhood vaccination programmes; internationally coordinated approaches; commitment to set up healthcare centres in remote areas; sustained campaign engagement from health bodies, communities, and funders; efficient distribution of health workers; innovations, new tools and well-managed programmes. Amongst several others, we can observe a similar bearing in the efforts of the Global Fund, an NGO that has invested more than US$17.9 billion in malaria control programs as of June 2023. [6]
Finally, as researchers continue to discover new novel vaccines to tackle malaria, there is hope for every “at-risk” child—in Africa and beyond. However, given the way things are, malaria cannot be eliminated with vaccines alone, but with all hands on deck.
References
[1] Max Roser (2022) – “Malaria: One of the leading causes of child deaths, but progress is possible and you can contribute to it” Published online at OurWorldInData.org. Retrieved 12 January 2024 from: ‘https://ourworldindata.org/malaria-introduction‘
[2] “WHO recommends R21/Matrix-M vaccine for malaria prevention in updated advice on immunization”. Retrieved 12 January 2024 from: https://www.who.int/news/item/02-10-2023-who-recommends-r21-matrix-m-vaccine-for-malaria-prevention-in-updated-advice-on-immunization
[3] Kurayi Mahachi et al. (02 September 2022) “Zero- or missed-dose children in Nigeria: Contributing factors and interventions to overcome immunisation service delivery challenges.” Retrieved 12 January 2024 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9485449/
[4] Valentine Duru, Benoit Witkowski, and Didier Ménard, (7 December 2016). “Plasmodium falciparum Resistance to Artemisinin Derivatives and Piperaquine.” Retrieved 12 January 2024 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5154433/
[5] Dorcas Wangira (12 January 2024) “Cape Verde reaches malaria-free milestone” Retrieved 12 January 2022 from https://www.bbc.com/news/world-africa-67951537
[6] Retrieved 12 January 2024 from https://www.theglobalfund.org/en/malaria/